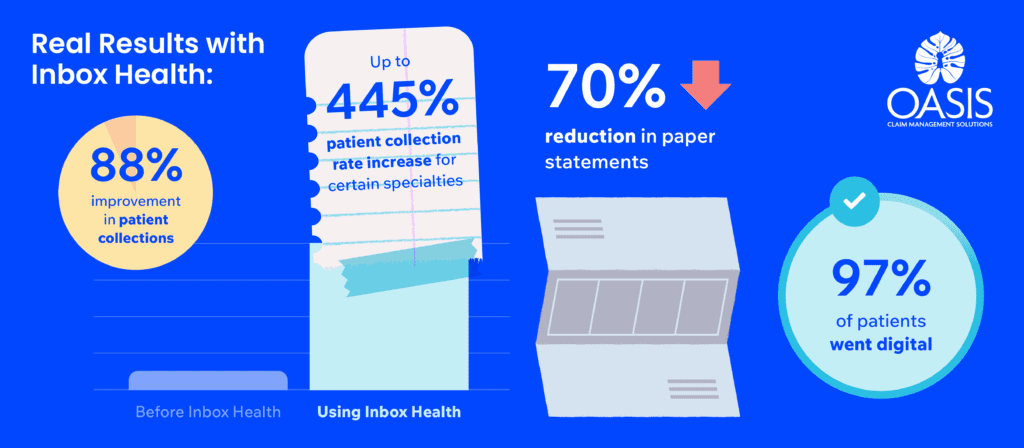
Michael Smith, CPA and CEO of Oasis Claim Management Solutions, did an analysis of his business in 2021 and determined that patient collections were an area that required attention. But where there is weakness there is opportunity, so he put a plan in motion to adopt the best solution to better manage patient A/R. With Inbox Health, patient collections have increased by 88%.
Michael’s analysis discovered opportunities to increase patient collections and the number of touchpoints for patient engagement. In the future, he predicted costs of paper statements were going to rise as well as the popularity to engage with patients over text and email platforms. When it came to evaluating solutions, he looked at four key elements:
- Patient engagement: Are the patient engagement tools easy to use? Is the solution secure without too many barriers to access?
- Biller efficiencies: Will the solution reduce the number of outbound calls my billing team makes tracking down patient payments?
- Call volume: Will the solution reduce the number of incoming calls?
- Revenue cycle strength: How many revenue cycles will run per month? What forms of payment are accepted? Are payment plans offered?
After evaluating multiple vendors, Inbox Health was the obvious choice, and his team felt the impact immediately.
“Inbox Health has helped us achieve all of our goals,” Michael says. “Before using Inbox Health, we were sending out patient statements once every 30 days. Now, we send statements up to five times per week and spend less time on the process. In many cases, we do not even send paper statements because patients pay so quickly digitally. It’s had a huge impact.”
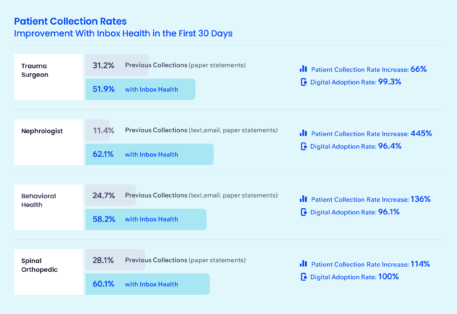
Patient A/R is often an overlooked opportunity for medical billers, but Michael sees his ability to optimize patient collections through Inbox Health’s platform a differentiator. On average, 14% to 18% of revenue from his accounts is tied to patient collections, a number that is starting to garner more attention from medical billers.
In addition to increasing the frequency of sending statements, Oasis has also seen an increase in collection rates and a 97% adoption rate of digital communication and payment. Live chat has helped cut down on phone calls from patients, and the company is reducing its carbon footprint by decreasing paper statements mailed by 70%. Many of Oasis’ patients are transient, so by enabling digital billing, collections are not interrupted with mail that is returned to sender. Even better, Inbox Health is able to intelligently flag errors in mailing addresses, allowing his billing team to rectify the error before a bill is sent.
“The patient experience starts at registration all the way through billing and payment. Customer service is important for practices that want to grow,” Michael says.
When Michael has conversations with current and prospective practices, he uses the analytics to increase the value of his services. “I am able to have conversations about the impact of patient collections that no one else is having,” Michael says.
About Oasis Claim Management Solutions

Name: Michael Smith
Role: CPA and CEO
Company: Oasis Claim Management Solutions
Location: Wheat Ridge, CO and Naples, FL
www.oascms.com
833.857.2088